Missing teeth affect more than just your appearance; they also impact your ability to eat, speak, and maintain jawbone health. If you’re exploring tooth replacement options, you’ve likely encountered two main implant solutions: full mouth and partial dental implants. Understanding the difference between these approaches is crucial for making an informed decision about your oral health.
Dental implants have revolutionized tooth replacement, offering a permanent solution that looks, feels, and functions like natural teeth. Whether you need to replace a few missing teeth or an entire arch, implant dentistry provides options tailored to your specific situation.
Understanding Dental Implant Basics
Before comparing full mouth and partial implants, it’s important to understand what dental implants are and how they work.
What Are Dental Implants?
Dental implants are titanium posts surgically placed into your jawbone to serve as artificial tooth roots. These posts integrate with your bone through a process called osseointegration, creating a stable foundation for replacement teeth. Unlike dentures or bridges, implants don’t rely on adjacent teeth or adhesives. They stand independently, preserving your natural bone structure.
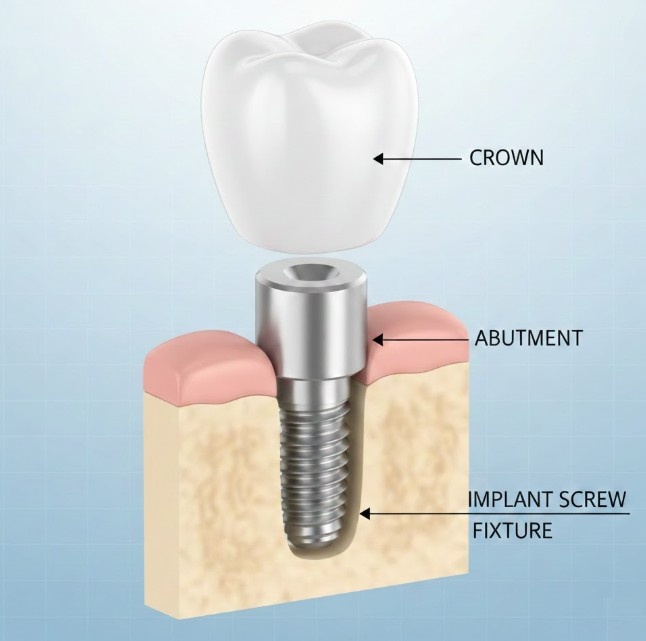
The implant system typically consists of three components: the implant post (placed in the jawbone), the abutment (connector piece), and the crown or prosthetic tooth (visible portion). This three-part design allows for customization based on your aesthetic needs and functional requirements.
Benefits of Choosing Dental Implants
Dental implants offer significant advantages over traditional tooth replacement methods:
- Bone preservation: Implants stimulate jawbone tissue, preventing the bone loss that occurs with missing teeth
- Natural appearance: Custom-designed crowns match your existing teeth in color, shape, and size
- Improved function: Restore full chewing capacity and clear speech
- Longevity: With proper care, implants can last 25 years or longer
- No impact on healthy teeth: Unlike bridges, implants don’t require grinding down adjacent teeth
- Enhanced confidence: Permanent teeth eliminate worries about slipping dentures or gaps in your smile
What Are Partial Dental Implants?
Partial dental implants replace one or more missing teeth while preserving your remaining natural teeth. This targeted approach addresses specific gaps in your smile without affecting healthy teeth.
Single Tooth Implants
When you’re missing just one tooth, a single dental implant provides the most conservative and effective solution. Your dentist places one implant post at the site of the missing tooth, attaches an abutment, and crowns it with a custom restoration. This standalone replacement integrates seamlessly with your natural teeth, maintaining proper spacing and bite alignment.
Single implants are ideal for isolated tooth loss caused by injury, decay, or congenital absence. They prevent neighboring teeth from shifting into the gap, a common problem that can create bite issues and increase cavity risk.
Implant-Supported Bridges
For replacing multiple consecutive missing teeth, an implant-supported bridge offers an efficient solution. Instead of placing an implant for each missing tooth, your dentist positions implants at either end of the gap to support a bridge of prosthetic teeth. For example, replacing three missing teeth might require only two implants with a three-unit bridge.
This approach reduces the number of surgical sites while still providing stable, permanent tooth replacement. Implant bridges function better than traditional bridges because they don’t rely on natural teeth for support, preserving the integrity of your remaining dentition.
Who Benefits Most from Partial Implants?
Partial dental implants work best for patients who:
- Have lost one or several teeth in specific areas
- Maintain good oral health in remaining teeth
- Have adequate jawbone density to support implants
- Want to preserve healthy teeth without alteration
- Seek a long-term solution that feels natural
- Need to restore chewing function in targeted areas
Candidates for partial implants should have healthy gums, sufficient bone volume, and a commitment to maintaining excellent oral hygiene. Your dentist at irvinecadentist.com can evaluate your specific situation through a comprehensive examination and imaging.
What Are Full-Mouth Dental Implants?
Full mouth dental implants replace all teeth in either the upper or lower arch (or both) using a strategic implant placement system. This comprehensive approach restores complete dental function when most or all natural teeth are missing, severely damaged, or failing.
All-on-4 Treatment Concept
The All-on-4 technique represents one of the most popular full-mouth restoration methods. This innovative approach uses just four strategically placed implants to support a complete arch of prosthetic teeth. The posterior implants are angled up to 45 degrees to maximize contact with available bone, often reducing or eliminating the need for bone grafting in patients with moderate bone loss. However, those with severe resorption may still require grafting before implant placement.
All-on-4 offers several advantages: fewer surgical sites, reduced treatment time, lower costs compared to individual implants, and often immediate loading with temporary teeth on the same day as surgery.
When adequate implant stability is achieved during surgery, typically measured by insertion torque, patients can receive temporary functional teeth the same day. However, immediate loading is not appropriate for all cases, and some clinicians may delay loading to protect the healing implants.
All-on-6 and All-on-8 Options
For patients with greater bone density or those seeking additional stability, All-on-6 and All-on-8 systems provide enhanced support. These methods use six or eight implants per arch, distributing chewing forces more evenly and potentially extending the longevity of the restoration.
The additional implants distribute chewing forces more evenly across the arch, reducing the load placed on each individual implant and improving long-term biomechanical stability. This makes All-on-6 and All-on-8 particularly beneficial for patients with higher bite forces or parafunctional habits such as bruxism.
Individual Implants for Full Arch Restoration
Some patients opt for individual implants throughout the entire arch, creating the most natural replacement pattern. This approach typically requires 6-10 implants per arch and results in fixed individual crowns rather than a connected prosthesis.
While more expensive and time-intensive, individual full arch implants offer maximum flexibility for maintenance and repair. If one crown or implant needs attention, the dentist can address it without affecting the rest of the restoration.
Who Needs Full Mouth Implants?
Full mouth dental implants serve patients who:
- Are missing all or most teeth in one or both arches
- Have extensive tooth decay or periodontal disease affecting multiple teeth
- Currently wear dentures but seek a permanent, stable solution
- Face extraction of the remaining compromised teeth
- Want to restore full chewing capacity and facial structure
- Need comprehensive rehabilitation after trauma or disease
Your dentist will assess bone quality, overall health, and lifestyle factors to determine if you’re a good candidate for full mouth restoration. Conditions like uncontrolled diabetes, active periodontal disease, or insufficient bone may require treatment before proceeding with implant surgery.
Schedule your personalized implant consultation and receive a detailed treatment plan tailored to your needs.
Contact the Best Irvine Dentist Now!
Key Differences Between Full-Mouth and Partial Implants
Understanding the distinctions between these two approaches helps clarify which option aligns with your dental needs and personal circumstances.
Number of Teeth Replaced
The most obvious difference lies in scope: partial implants replace specific missing teeth while preserving healthy natural teeth, whereas full mouth implants replace an entire arch of teeth. Partial solutions might involve one to several implants, while full mouth restorations typically use four to ten implants per arch to support complete dentures or bridges.
This fundamental difference affects every aspect of treatment planning, from surgical approach to prosthetic design.
Treatment Complexity and Timeline
Partial implant procedures are generally less complex, involving fewer surgical sites and shorter appointment times. A single tooth implant might require 3-6 months from initial surgery to final crown placement, with most of that time dedicated to healing and osseointegration.
Full mouth implant treatments involve more extensive planning, including detailed imaging, treatment simulations, and coordination between surgical and restorative phases. However, modern techniques like All-on-4 can sometimes deliver functional teeth in a single day, though the permanent prosthesis still requires several months of healing.
Complete full mouth restoration typically spans 3–8 months for straightforward cases. When preparatory procedures such as sinus lifts, ridge augmentation, or block bone grafts are required, total treatment time can extend to 12–18 months, as grafted bone must fully mature before implants can be placed.
Investment Considerations
Partial implants require lower upfront investment since they address limited areas. A single tooth implant represents a moderate expense, while multiple partial implants increase costs proportionally.
Full mouth implants involve higher initial costs due to the comprehensive nature of treatment, multiple implant placement, and complex prosthetics. However, when compared to placing individual implants for every missing tooth, techniques like All-on-4 offer considerable value. Many patients find that the long-term benefits, eliminating ongoing denture adjustments, adhesives, and replacements, make full mouth implants a sound investment.
Recovery and Adjustment Period
Recovery from partial implant surgery is typically straightforward, with discomfort limited to the surgical site. Most patients return to normal activities within a few days, managing any discomfort with over-the-counter pain relievers.
Full mouth implant surgery involves more extensive intervention, potentially requiring stronger pain management and a longer initial recovery period. Swelling and bruising may be more pronounced, and dietary restrictions last longer as multiple surgical sites heal. However, many patients report that the immediate improvement in function and appearance makes the recovery period worthwhile.
Adjustment to partial implants is minimal since they integrate with existing teeth. Full mouth prosthetics require more adaptation as patients learn to speak and eat with completely new teeth, though most adjust within a few weeks.
Maintenance Requirements
Both partial and full mouth implants require diligent oral hygiene, but the specific care protocols differ slightly.
Partial implants demand careful cleaning around each implant site, using techniques similar to caring for natural teeth: brushing, flossing, and potentially using interdental brushes. Regular dental cleanings ensure the implants and surrounding gums remain healthy.
Full mouth implants require specialized cleaning techniques depending on the prosthetic design. Fixed prosthetics may need water flossers or specialized floss threaders to clean beneath the restoration. Your dental team will provide detailed instructions for maintaining your specific implant system.
Most implant patients follow a standard recall schedule of every 6 months, though your dentist may recommend more frequent visits, typically every 3-4 months, if you have a history of periodontal disease, peri-implantitis, or other risk factors that require closer monitoring.
How to Determine Which Option Is Right for You
Choosing between full mouth and partial implants depends on multiple factors unique to your oral health situation and personal preferences.
Assessing Your Current Dental Health
Your existing dental condition serves as the primary determining factor. Consider:
For partial implants: You have healthy teeth worth preserving, isolated gaps from tooth loss, and good bone density in affected areas. Your remaining teeth have solid structure without extensive decay or severe periodontal disease.
For full mouth implants: Most teeth are compromised by decay, disease, or damage. Remaining teeth require extensive treatment, or you currently struggle with ill-fitting dentures. Multiple teeth are failing or missing throughout the arch.
A comprehensive dental examination, including X-rays and potentially 3D CT scans, reveals bone quality, gum health, and the viability of existing teeth. Your dentist evaluates whether preserving remaining teeth is practical or if extraction and full arch restoration provide better long-term outcomes.
Bone Density and Quality Considerations
Adequate jawbone volume is essential for successful implant integration. When teeth are missing for extended periods, the surrounding bone deteriorates, a process called resorption.
Partial implants require sufficient bone at specific sites where teeth are missing. If bone loss has occurred, localized bone grafting can rebuild the area before implant placement.
Full mouth implants address more extensive bone loss through strategic implant angles (as in All-on-4) or comprehensive bone grafting when necessary. Patients with significant bone deterioration might actually be better candidates for full mouth solutions that work around bone deficiencies rather than multiple partial grafts.
Bone density testing through CBCT imaging provides precise measurements, allowing your dentist to recommend the approach most likely to succeed given your anatomy.
Lifestyle and Functional Goals
Consider how you want your restored smile to function in daily life:
Choose partial implants if you: Need targeted replacement for specific activities (like chewing on one side), want to maintain your natural bite pattern, prefer conservative treatment affecting minimal areas, or have recently lost teeth and want immediate replacement.
Consider full mouth implants if you: Struggle with current dentures during eating or speaking, want to eliminate denture adhesives and daily removal, need comprehensive facial support to restore a youthful appearance, or desire the confidence of permanently fixed teeth.
Your expectations about eating, speaking, and smiling influence which solution provides the most satisfaction. Full mouth restorations offer dramatic transformations, while partial implants preserve what’s working while fixing specific problems.
Consulting with Your Implant Dentist
Schedule a comprehensive consultation with an experienced implant dentist to discuss your options thoroughly. During this appointment, expect:
- Detailed examination of teeth, gums, and bone structure
- Review of your medical history and any conditions affecting healing
- Discussion of your goals, concerns, and preferences
- Explanation of recommended treatment options with visual aids
- Review of treatment timeline and what to expect at each stage
- Questions about aftercare and long-term maintenance
Don’t hesitate to ask questions about success rates, potential complications, and what happens if problems arise years later. A qualified implant dentist provides honest assessments about which approach offers the best combination of function, aesthetics, and longevity for your situation.
Not sure whether full mouth or partial implants are right for you? A detailed evaluation can help you understand your options clearly and confidently.
Get a Personalized Implant Assessment
The Treatment Process: What to Expect
Understanding the treatment journey helps you prepare mentally and practically for your implant procedure, whether partial or full mouth.
Initial Consultation and Planning
Your implant journey begins with a comprehensive evaluation. Your dentist examines your mouth, takes detailed X-rays or 3D CBCT scans, and discusses your medical history. These diagnostics reveal bone quality, nerve locations, sinus positions, and the condition of existing teeth.
For full mouth cases, digital treatment planning software may create a virtual simulation showing how your new smile will look. Some practices offer same-day imaging and prosthetic design, allowing you to see your projected results before committing to treatment.
Your dental team develops a customized treatment plan outlining each step, from any preparatory procedures through final restoration. You’ll receive information about timeline expectations, healing requirements, and what happens at each appointment.
Surgical Procedure Details
On surgery day, your dentist administers local anesthesia to ensure comfort throughout the procedure. Many practices offer sedation options for anxious patients or extensive cases.
For partial implants, the surgeon creates a small incision in the gum tissue, prepares a precise site in the jawbone, and places the titanium implant. The gum is sutured closed over or around the implant. The entire process for a single implant typically takes 1-2 hours.
Full mouth procedures follow similar principles but involve multiple implant placements in one session. The surgeon may extract any remaining compromised teeth before placing implants. Strategic positioning ensures optimal load distribution and stability. When immediate loading is appropriate, temporary teeth can attach the same day, minimizing time without teeth.
Healing and Osseointegration Phase
After surgery, osseointegration begins, the biological process where bone cells grow onto the implant surface, fusing it securely to your jaw. This crucial phase typically requires 3-6 months for complete integration.
During healing, you’ll follow specific care instructions: a soft food diet, gentle cleaning around surgical sites, avoiding smoking or tobacco use, taking prescribed medications, and attending follow-up appointments to monitor progress.
Smoking is one of the most significant lifestyle risk factors for implant failure, as it restricts blood flow during the critical osseointegration phase.
For partial implants, temporary crowns may protect the site while allowing function. Full-mouth patients with immediate load prosthetics use temporary teeth designed to distribute forces carefully during the healing period.
Final Restoration Placement
Once osseointegration is complete, you return for final restoration. For partial implants, your dentist uncovers the implant (if buried during healing), attaches the abutment, and takes impressions for your permanent crown or bridge. After fabrication in a dental laboratory, the restoration is secured to the implant, completing your treatment.
Full-mouth patients receive their permanent prosthesis after healing is confirmed. The dentist attaches the final bridge or denture, makes any necessary adjustments for comfort and appearance, and provides detailed care instructions.
The transition to your permanent teeth marks the beginning of your long-term relationship with your implants, one that requires ongoing care to ensure lasting success.
Missing teeth don’t have to limit your comfort or confidence. Discover a long-term solution designed around your goals, health, and lifestyle.
Schedule Your Implant Consultation Today
Long-Term Success and Maintenance
Dental implants offer exceptional longevity, but their success depends significantly on proper care and regular professional monitoring.
Oral Hygiene for Implants
Maintaining implants requires diligent daily care similar to natural teeth:
Brushing: Use a soft-bristled toothbrush twice daily, paying special attention to where the implant meets the gum tissue. Electric toothbrushes with pressure sensors help prevent damage to prosthetic teeth.
Flossing: Clean between implants and around abutments daily using unwaxed floss, implant-specific floss, or water flossers. For full mouth prosthetics, specialized floss threaders access areas beneath bridges.
Antimicrobial rinse: Your dentist may recommend alcohol-free antimicrobial mouthwash to reduce bacterial accumulation around implants.
Avoid harmful habits: Don’t chew ice, hard candies, or other substances that could damage prosthetic teeth. If you grind your teeth, wear a protective nightguard.
Professional Monitoring and Care
Regular dental visits are essential for implant longevity. Most implant patients follow a standard recall schedule of every 6 months. Your dentist may recommend more frequent visits, typically every 3-4 months, if you have a history of periodontal disease, peri-implantitis, or other risk factors requiring closer monitoring.
During these visits, your hygienist uses specialized instruments that won’t scratch implant surfaces. Your dentist examines implant stability, checks for signs of infection or bone loss, evaluates the condition of prosthetic teeth, and takes periodic X-rays to monitor bone levels around implants.
Professional monitoring catches potential problems early when they’re most treatable. Peri-implantitis, inflammation and infection around implants, can lead to implant failure if undetected, but regular care prevents most cases.
Expected Lifespan of Dental Implants
With proper care, dental implant posts can last 25 years or more, often a lifetime. The prosthetic components (crowns, bridges) typically require replacement every 10-15 years due to normal wear, though many last longer with careful maintenance.
Dental implants consistently demonstrate high success rates in peer-reviewed literature, with many studies reporting rates above 95% at 10 years for healthy patients. Rates can vary based on implant location, the patient’s systemic health, bone quality, and oral hygiene practices, so individual outcomes may differ.
Factors affecting longevity include:
- Oral hygiene practices
- Tobacco use (significantly increases failure risk)
- Overall health conditions like diabetes
- Bone quality and quantity
- Proper bite distribution
- Professional maintenance frequency
Full mouth implant systems show similar success rates, with the prosthetic components sometimes requiring adjustments or repairs over time while the implant posts remain solidly integrated.
Investing in quality initial treatment and committing to ongoing care ensures your dental implants provide decades of reliable function.
Frequently Asked Questions
How painful is dental implant surgery?
Most patients report minimal discomfort during dental implant surgery due to effective local anesthesia. During the procedure, you’ll feel pressure but no pain. Post-operative discomfort is typically manageable with over-the-counter pain relievers and usually subsides within 3-7 days. Many patients compare the experience to having a tooth extraction, temporary discomfort followed by progressive improvement. Full mouth procedures may involve more initial soreness, but most patients find the results well worth any temporary inconvenience.
Can I get dental implants if I have bone loss?
Yes, bone loss doesn’t necessarily disqualify you from dental implants. Your dentist may recommend bone grafting to rebuild the jaw before implant placement, or use techniques like All-on-4 that work with available bone. Advanced imaging helps determine if you have sufficient bone in strategic locations. Some full mouth solutions actually work better for patients with bone loss than attempting multiple partial implants, as angled placement and strategic positioning maximize contact with existing bone structure.
How long does the entire implant process take?
The timeline varies by treatment type. Single partial implants typically require 3-6 months from initial surgery to final crown placement, with most time dedicated to healing. Full mouth implants may provide temporary teeth immediately, with permanent restoration following 3–8 months of healing for straightforward cases, or longer if bone grafting is required before implant placement. Factors affecting the timeline include individual healing capacity, whether bone grafting is needed, and the specific technique used. Some modern protocols compress timelines significantly, while complex cases require additional time for optimal results.
Will my dental insurance cover implants?
Dental insurance coverage for implants varies significantly by plan. Some policies cover a portion of implant treatment, classifying it as major restorative work with 50% coverage after deductibles. Others exclude implants entirely or only cover certain components. Medical insurance may contribute if tooth loss resulted from an accident or disease. Many dental practices offer financing options to make treatment accessible. Contact your insurance provider for specific coverage details, and discuss payment options during your consultation at Irvine CA Dentist.
What are the risks of dental implant surgery?
Dental implant surgery is safe with high success rates, but like any surgical procedure, it carries some risks. Potential complications include infection at the surgical site, injury to surrounding teeth or blood vessels, nerve damage causing numbness or tingling (rare), sinus problems when upper jaw implants protrude into sinus cavities, and implant failure if osseointegration doesn’t occur. Most complications are preventable through proper planning, skilled surgical technique, and following post-operative care instructions. Choosing an experienced implant dentist significantly reduces risk.
Can dental implants be removed if needed?
While dental implants are designed as permanent solutions, they can be removed if necessary due to infection, failure, or other complications. Removal requires a surgical procedure to separate the integrated implant from the surrounding bone. However, the vast majority of implants remain successful for decades without the need for removal. If a crown or bridge on an implant fails, the restoration can typically be replaced without disturbing the underlying implant post itself.
Taking the Next Step Toward Your New Smile
Choosing between full mouth and partial dental implants represents an important decision about your oral health and quality of life. Both options offer significant advantages over traditional tooth replacement methods, providing stability, function, and natural appearance that transform daily activities like eating and speaking.
Partial dental implants excel when you need targeted tooth replacement while preserving healthy natural teeth. They offer conservative treatment that addresses specific gaps without unnecessary intervention. Full mouth dental implants provide comprehensive restoration for patients with extensive tooth loss or failing dentition, delivering dramatic improvements in function and facial aesthetics through efficient implant placement techniques.
Your unique situation, including the number of missing teeth, bone quality, overall health, lifestyle goals, and budget, determines which approach offers the best outcomes. No single solution works for everyone, which is why personalized assessment by an experienced implant dentist is essential.
Modern dental implant techniques have made tooth replacement more predictable, comfortable, and accessible than ever before. Whether you need one implant or a full mouth transformation, today’s implant dentistry can restore your confidence and oral function for decades to come.
Ready to explore your implant options? Schedule a comprehensive consultation at irvinecadentist.com to receive a personalized treatment plan, detailed timeline, and clear answers to all your questions about partial or full mouth dental implants.
Your journey toward a complete, confident smile begins with understanding your options, and we’re here to guide you through every step.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always follow your dentist’s specific post-operative instructions, as individual care recommendations may vary based on your unique situation.
